Published March 6, 2026
In the early 1980s, the U.S. experienced a public reemergence of hunger — not because the country lacked food, but because federal policy choices tightened the “last-resort” systems that had helped Americans with low incomes weather recessions. The Reagan administration took office amid rising economic strain and subsequently pursued a broad package of tax breaks for the wealthy, along with cuts, reductions, and eligibility restrictions across low-income economic mobility programs, including the Food Stamp Program (now the Supplemental Nutrition Assistance Program, SNAP). Those changes landed while unemployment and poverty were climbing, creating a predictable mismatch: need increased, but assistance became harder to access and less adequate.
Congress enacted many of these changes through early 1980s budget reconciliation. Proposed and enacted rules emphasized expenditure control by narrowing eligibility, delaying benefit adjustments, and limiting deductions that recognize real household costs. For food assistance, the policy direction moved toward an absolute gross-income cutoff in addition to the net income test, with fewer allowances for households with unavoidable high expenses, such as medical costs. The result was not simply smaller benefits; it was a structural shift that pushed some households out of eligibility and reduced support for others precisely when their purchasing power and material hardship were worsening.
Because the Reagan administration denied that hunger was an issue and lacked a comprehensive, real-time nutrition surveillance system, clinicians, mayors, and advocates tried to measure what was happening through a patchwork of field investigations and surveys. Beginning in 1982, local providers and physicians reported growing numbers of families who could not reliably obtain enough food. A bipartisan national survey by the U.S. Conference of Mayors described hunger as a “most serious emergency,” and major cities treated it like a disaster-level problem requiring urgent response. In parallel, medical and public-health leaders organized direct investigations into hunger and malnutrition.
Below is a snapshot of that national evidence base:
Selected National Hunger and Emergency Food Studies (1982–1984)
Study / Report Title | Organization | Date |
Survey of U.S. Cities on Hunger and Emergency Food Needs | United States Conference of Mayors | October 1982 |
National Hunger Report | United Church of Christ | January 1983 |
Case Studies of Emergency Food Programs | U.S. Department of Agriculture | May 1983 |
Soup Lines and Food Baskets | Center on Budget and Policy Priorities | May 1983 |
Hunger in American Cities | United States Conference of Mayors | June 1983 |
National Emergency Assistance/ Hunger Report | The Salvation Army | June 1983 |
Public and Private Efforts to Feed America’s Poor | U.S. General Accounting Office | June 1983 |
Domestic Hunger and Poverty Report | National Council of Churches | August 1983 |
Hunger Watch | Bread for the World | September 1983 |
Responses to Urban Hunger | United States Conference of Mayors | October 1983 |
Food Research & Action Center | November 1983 | |
American Hunger | Harvard School of Public Health | February 1984 |
Hard Choices for Hungry Families | Save the Children/American Can Company | September 1984 |
The Urban Poor and the Economic Recovery | United States Conference of Mayors | September 1984 |
Food Research & Action Center | November 1984 |
These ad hoc efforts consistently pointed in the same direction: Hunger and food hardship were rising, and vulnerable groups — especially children and older adults — faced heightened risk of nutrition-related harm. Medical investigators emphasized outcomes that do not always look like famine but still carry serious health costs: child growth faltering, low birth weight, and other pediatric impacts linked to inadequate nutrition; and undernutrition interacting with chronic disease among older adults. The core problem was not a mystery or individual failure; it was the systems design. When policymakers constrain benefits eligibility, suppress benefit adequacy, and add administrative friction, the predictable downstream effect is more untreated food hardship, more reliance on emergency food, and more preventable health deterioration.
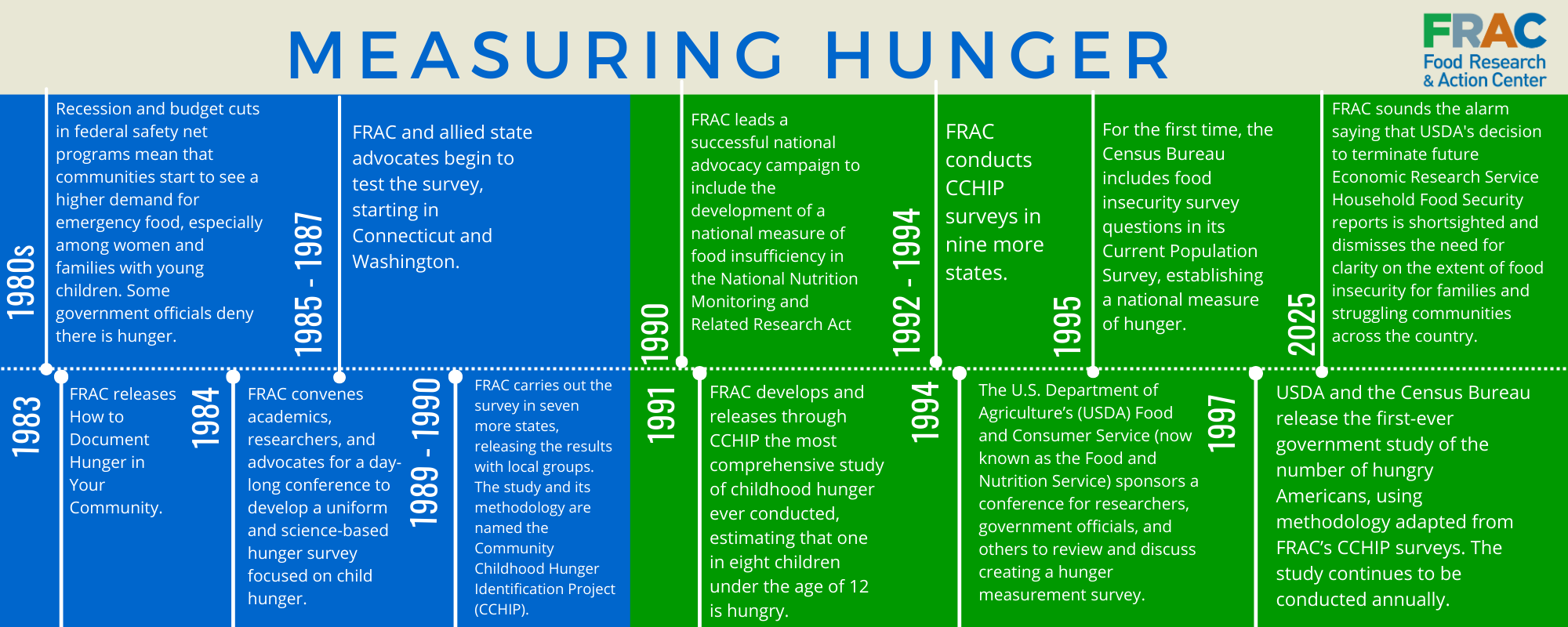
That history explains why objective measurement became central to effective anti-hunger policy. FRAC created the first comprehensive study of childhood hunger, called the Community Childhood Hunger Identification Project (CCHIP), and that work prompted USDA and the Census Bureau to add food security questions to national surveys. Building on this foundation, in the mid-1990s, the federal government developed a durable measurement tool by fielding the Food Security Supplement to the Current Population Survey (FSS), starting in April 1995, to capture food hardship across a range of severity and enable consistent trend reporting. USDA’s Economic Research Service has used CPS-based food security data to publish annual national estimates for decades. This infrastructure matters because it makes policy impacts visible: It allows the country to detect when hardship rises, identify which groups bear the brunt, and connect policy changes to measurable consequences for child development and older-adult health.
The Reagan-era lesson is straightforward: When policymakers cut eligibility and adequacy while hardship rises, hunger grows — and in the absence of standardized surveillance, the nation defaults to delayed, fragmented recognition, documented only after clinicians, mayors, and foundations scramble to fill the evidence gap. A modern food security supplement exists precisely to prevent that failure mode. When government weakens or eliminates that objective system, it also weakens the public’s ability to evaluate whether policy is increasing malnutrition risk, growth failure among children, and diet-sensitive disease burdens among older adults.
Take Action
In 2024, the total cost of the Food Security Supplement to the Current Population Survey was just over $1 million dollars, and that year included new methodological research. In many years, the cost has been substantially lower (just $710,000 in 2022). To put the cost into perspective, it is similar to the cost of a cross-country flight on Air Force One (which is estimated to cost about $1 million based on reported hourly operational costs of $177,843). That small amount of funding for data collection informs more than $100 billion dollars in Supplemental Nutrition Assistance Program funding, as well as billions of additional dollars in state and local hunger-abatement programs.
1. Reach out to your Member of Congress and ask them to cosponsor the Food Assurance and Security Act by U.S. Reprs. Wesley Bell (D-MO) and Nanette Diaz Barragan (D-CA) to reinstate USDA’s Household Food Security Report.
2. On February 23, 2026, USDA issued a Request for Information to gather feedback on its statistical data, research, and economic analysis provided by ERS, NASS, and the Office of the Chief Economist. The deadline for comments is April 9, 2026. Join FRAC in submitting official comments to advocate for the reinstatement of the FSS report. A comment template is available for use.
3. While federal advocacy continues to restore the FSS, states can also follow California’s lead by filing state legislation and implementing a state version of the FSS until the federal FSS resumes.
4. Continue to challenge the false idea that the data in the FSS is duplicated or redundant. Refer to FRAC’s blog on, Threats to Food Security Data: Why the ‘Redundancy’ Claim Doesn’t Hold Up, for more details on how other surveys compare to CPS-FSS. No other survey offers the same timely insights as the Food Security Supplement at the national, state, and subgroup levels.

